Prisma Health: How a Diabetic Retinopathy Telemedicine Program Saved Eyesight in South Carolina

KEY METRICS
8.9K+ 1.2K+ 966+
Eye exams performed Patients With Identified Pathology Patients with Identified Diabetic Retinopathy
Prisma Health is South Carolina’s largest not-for-profit health organization, serving a diverse population of over 1 million patients across the state. Prisma Health services 21 counties, running 18 hospitals and over 300 physician practice sites. Prisma Health looks to transform the healthcare experience by expanding access to care and increasing education and research.
THE CHALLENGE:
Recognizing the staggering metric of 12 million people diagnosed with diabetic retinopathy, Prisma Health aimed to improve its offerings to ensure care for the whole patient.
The wide-reaching South Carolina health system had what they considered a “fragmented approach” to eye care. Meaning, without any in-office capabilities, they could only offer referrals out to eye care services.
This system quickly revealed many barriers to proper and comprehensive care, including annual diabetic retinopathy exams (DRE) for diabetic patients. Some of the barriers present in Prisma Health’s system included:
- Patients without insurance coverage were less apt to visit an eye doctor outside of the primary care setting due to costs.
- Access to eye care was sparse in certain areas.
- If a patient did end up seeing an outside eye doctor, Prisma Health struggled to receive results from that visit to integrate into the patients’ medical records. Staff found they spent valuable time tracking down the necessary reports from referrals.
All of this resulted in poor performance in diabetic retinopathy exam compliance across the board. In 2016, Prisma Health received a concerningly low compliance HEDIS measure of 30%. This lack of diabetic retinopathy exam compliance put diabetes patients at direct risk of blindness and vision loss and took away financial incentives from the organization.
Recognizing the urgency, Prisma Health set out to overhaul their fragmented system to better serve their large population of patients at risk for diabetic retinopathy.
THE SOLUTION:
Prisma Health began looking for an in-house diagnostic solution to improve patient outcomes and raise diabetic retinopathy exam compliance. They needed an approach that went hand-in-hand with operations to ensure all logistical issues were addressed and provided a consistent standard of care for at-risk patients in the primary care setting.
Prisma Health partnered with IRIS, an FDA Class II retinal telemedicine platform developed to help end preventable blindness caused by diabetic retinopathy. Prisma Health was able to partner with IRIS in this mission and begin the process of implementing a large-scale telemedicine platform for diabetic retinopathy exams.
Beginning early 2018, Prisma Health deployed the IRIS solution at four sites to establish proof of concept. 2019 became a building year, and IRIS soon scaled to reach nearly 20 primary care clinics across the state through a phased roll-out strategy. Today, Prisma Health has 44 sites participating in the IRIS program.
In partnering with IRIS, Prisma Health launched a new workflow that allowed patients to receive both a diabetic retinopathy exam in-house and an integrated diagnosis within one business day.
Instead of having to refer patients to outside eye care providers, IRIS provided a fully integrated and end-to-end solution. The diabetic retinopathy exam process at Prisma Health now follows the following structure:
- In-house exam: The diabetic retinopathy exam itself only takes moments and can be captured easily by any trained staff. Performing a diabetic retinopathy exam with IRIS does not require licensure or advanced medical training, so Prisma Health enabled medical assistant staff to administer the exams.
- Image Upload and Enhancement: The image taken during the diabetic retinopathy exam is then uploaded to the cloud-based platform. IRIS’s software enhances the image, and it is sent out to a board-certified ophthalmologist or retina specialist for review.
- Diagnosis: After receiving the enhanced image through the cloud, the interpreting physician remotely diagnoses the images for diabetic retinopathy or other suspected conditions.
- Referral: Diagnoses are returned through the same system and integrated directly into the patient’s chart through Prisma Health’s Epic EMR interface. At this time, any necessary referrals for treatment are also made.
This bidirectional workflow is due to IRIS’s ability to launch functionality through EHRs, like Prisma’s Epic interface. With integration through Epic, everything from flagging the patient for an IRIS exam, to receiving the diagnostic results is simplified and streamlined.
This simplified process empowered patients to complete their annual diabetic retinopathy exam and established a consistent – and accessible – standard of care.
THE RESULTS:
Closing Care Gaps:
- 8,904 Exams Performed To Date.
- 1,271 Patients With Identified Pathology — Diabetic Retinopathy or Otherwise.
Other suspected diseases include early and late-stage AMD, glaucoma, cataract, epiretinal membrane, and other ocular pathologies.
- 966 Patients with Identified Diabetic Retinopathy
- 553 IRIS Saves
Identified patients with severe or proliferative retinopathy, stages that are the highest threat to loss of eyesight.
- 1,142 Patients with RAF Eligible Diagnoses
- 96% overall gradability rating. A gradable image is one that is high quality enough to be diagnosed by an IRIS Reading Center Physician. While the majority of IRIS clients maintain high gradability rates, Prisma Health’s overall rate of 96% is especially impressive considering their exclusive use of handheld cameras.
*Data updated 9/28/2021
IRIS Impact on HEDIS quality scores at Prisma Health:
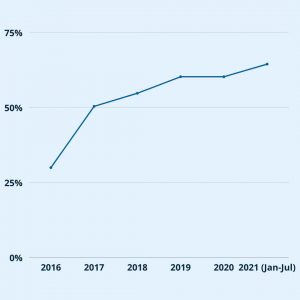
As Prisma Health continues to equip additional locations with the IRIS Solution, their HEDIS quality performance has also improved significantly.
THE IMPACT:
The fight to end preventable blindness addresses so many areas beyond diagnosis. As diabetic retinopathy progresses, therapies become aggressively more expensive, and blindness in adults puts financial, socioeconomic, and other costly burdens on the healthcare system, the community, and most importantly, the patient.
For example, the cost of retinal drug therapy is now the second most expensive pharmaceutical drug group behind cancer treatments. Early detection results mean the possibility for early treatment with less expensive therapies.
An annual diabetic retinopathy exam is an essential step in catching diabetic retinopathy in the earliest stages possible. Removing as many barriers as possible to this exam is crucial for patient compliance and closing care gaps.
Not only does early detection benefit the patient financially, but it can also lower costs for the healthcare systems that implement DRE integrations.
Prisma Health found the fee for service revenue (FFS) alone covered the cost of the IRIS program. On top of that, they were able to generate additional revenue through HEDIS bonuses and incentives as a result of increased compliance scores. HCC and RAF-related documentation also improved, helping to more accurately adjust their risk-based payer contracts.
The downstream repercussions of late diabetic retinopathy detection are expensive, and importantly, preventable. By removing all barriers to early DR detection, patients and healthcare systems can save sight and cut costs.
BUILDING AN EFFECTIVE DIABETIC RETINOPATHY EXAM PROGRAM:
An effective telemedicine program for diabetic retinopathy begins with education.
At Prisma Health, this meant teaching medical assistants how to discuss the diabetic retinopathy exam process with diabetes patients.
It was important to communicate with patients not only the importance of the exam but the benefits that came with receiving it through primary care. This included financial coverage, preventing additional doctor visits, ease of exam, and the low chance of dilation.
On the administrative side, Prisma Health found that it was important to approach diabetic retinopathy integration with an expectation that the process would be gradual. Roll out for telemedicine is never immediate, and should be intentionally paired with education and step-by-step workflow integration. This is all to ensure a sustainable and viable DR program.
Prisma Health also found that encouraging buy-in was crucial to roll out initiatives. Once their sites began to see results, they then identified champions of the program to continue the momentum forward.
REACHING EVERY PATIENT:
“It’s not just those patients that you assume have diabetic retinopathy because they already had complications from their diabetes…it’s not just those who you surround with services and resources because their diabetes has been out of control. Instead, it’s the patient that is silent. The patient that has diabetes with silent disease with no history of eye disease with mild to moderate diabetic control (Hgba1c) that we still need to worry about. The IRIS Solution makes it possible. I have been amazed by the level of retinal pathology found in our diabetic patient population, we call them IRIS sight saves!” — Dr. Nick Patel, Chief Digital Officer, Prisma Health

Prisma Health Team
Working with IRIS, Prisma Health was able to empower all of their diabetes patients to take control of their eye health, especially those with no previous indicators of diabetic retinopathy.
By expanding access and ease of exam, IRIS and Prisma Health closed care gaps and boosted compliance across their South Carolina health network. And, most importantly, they were able to keep the patient at the center of their care while helping to end preventable blindness amongst their diabetic population.
Book your demo today to see how you can easily integrate IRIS’s technology into your practice today.
SM073 Rev A.
Get started with IRIS today.
Want to know if IRIS is right for you? Schedule a one-on-one consultation with our team. We’re here to help.